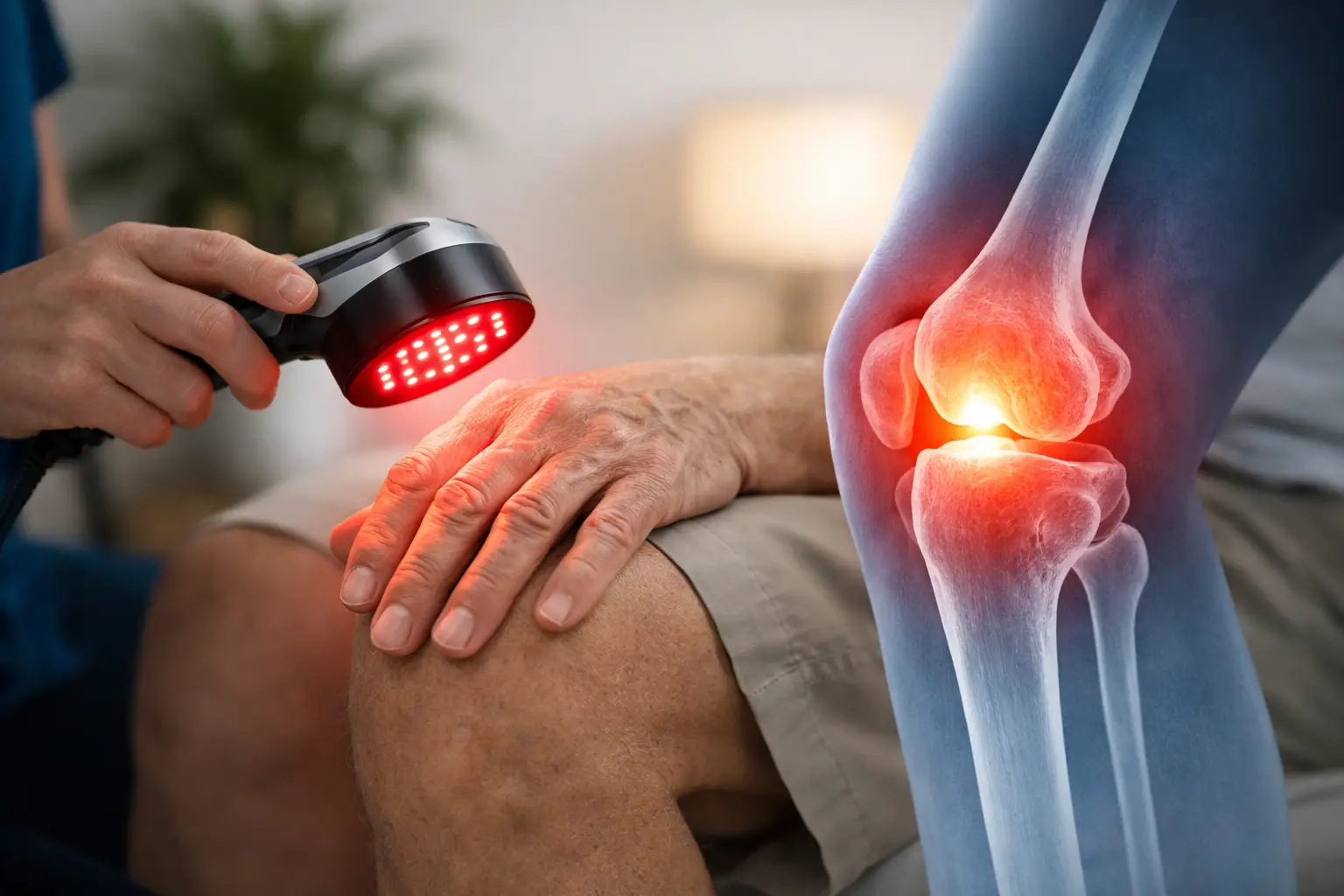
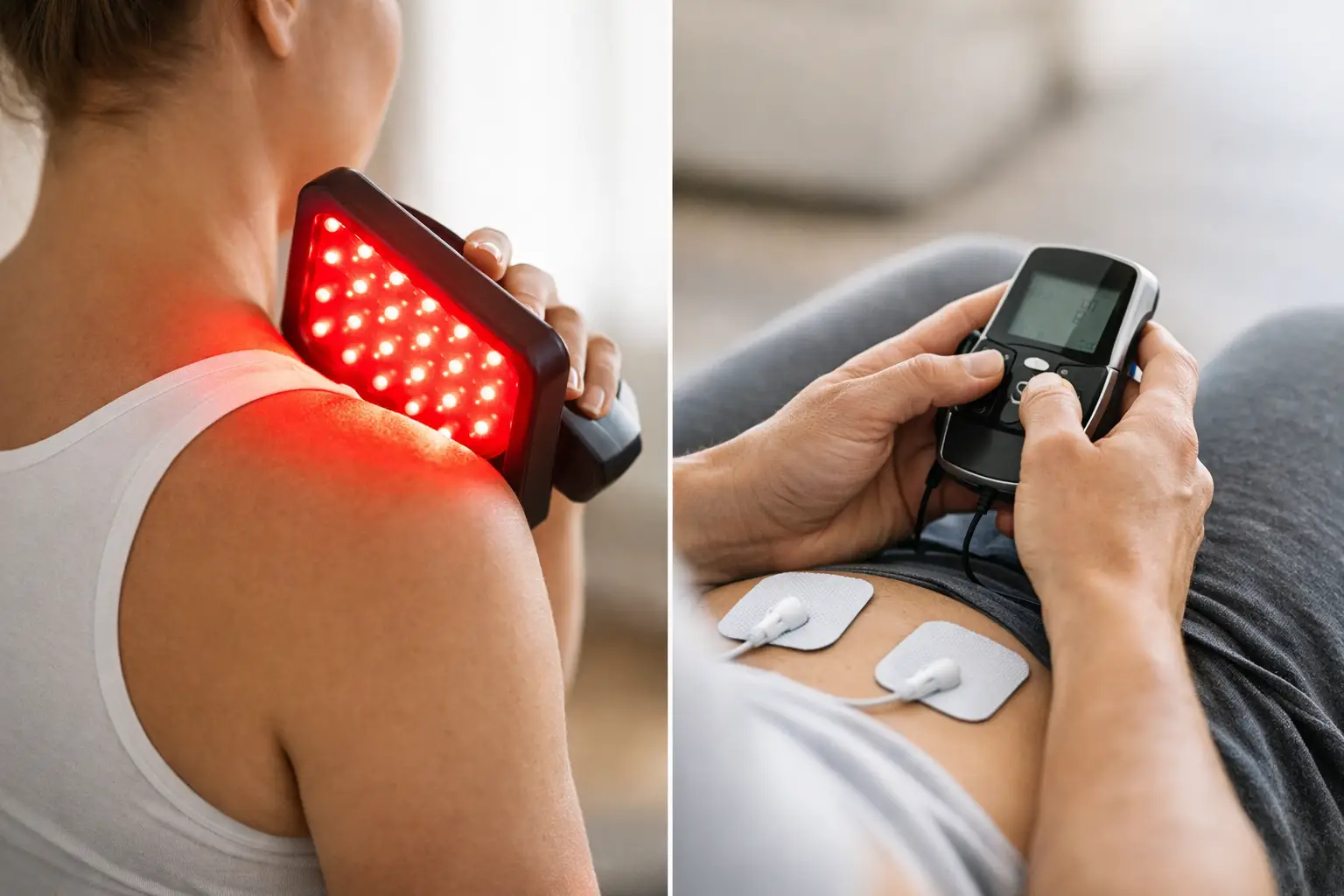
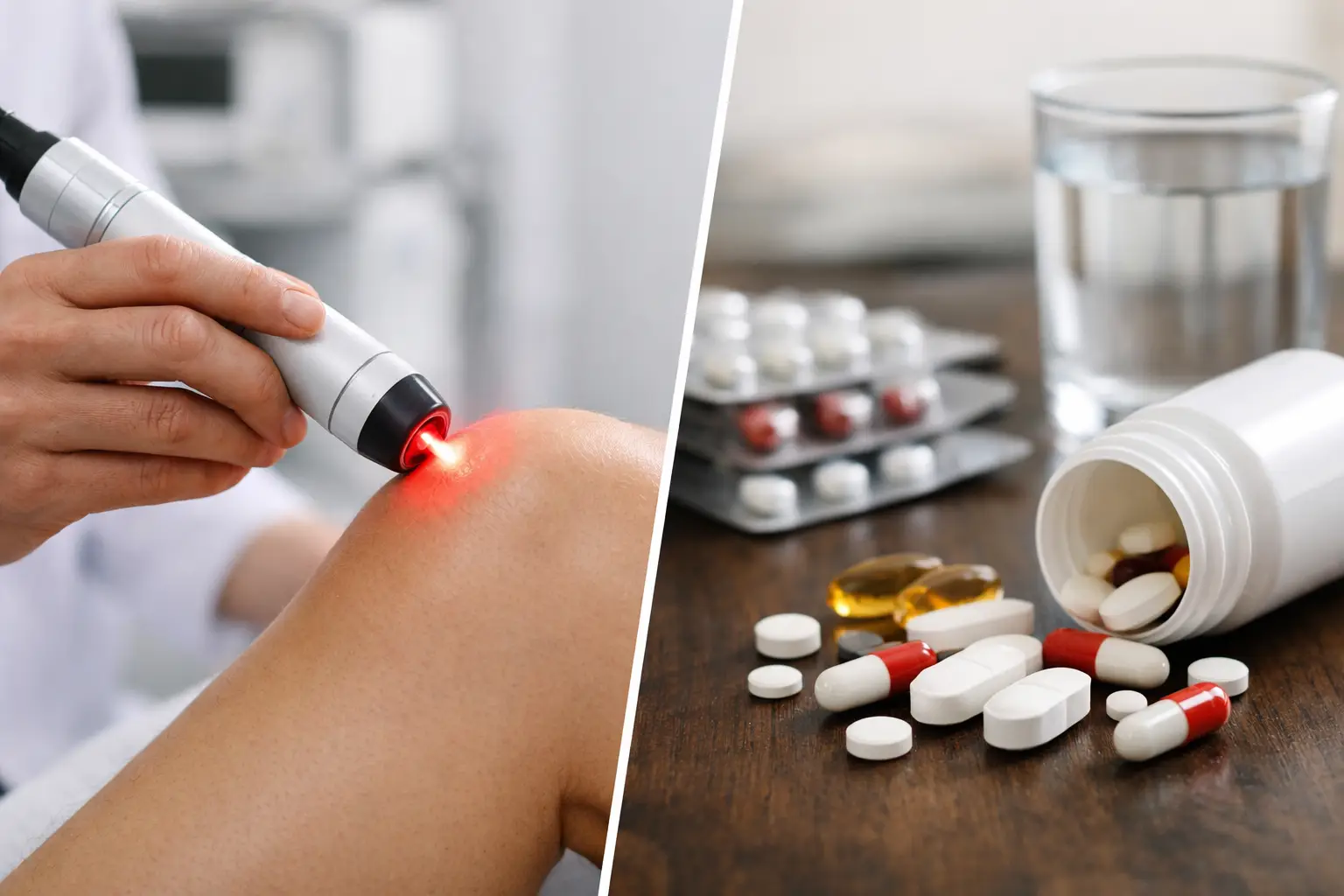
That first stiff step in the morning tells the story fast. Arthritis does not just show up as pain – it can change how you move, how long you stay active, and how confident you feel doing everyday things. So when people ask, can light therapy help arthritis, they are usually asking a bigger question too: is there a way to feel better without leaning harder on medications or giving up the activities they love?
For many people, low level light therapy is worth serious attention. It is non-invasive, drug-free, and easy to use at home or as part of a recovery routine. It is not a magic fix, and it does not reverse joint damage. But for the right person, used consistently, it may help reduce discomfort, calm inflammation, and improve mobility enough to make daily life feel more manageable again.
Can light therapy help arthritis in real life?
Yes, it can help some people with arthritis, especially when the goal is symptom relief rather than a cure. Light therapy is most often used to support reduced pain, less stiffness, and better joint function. That matters whether you are trying to open a jar, get through a workout, or simply walk without dreading the next step.
The key is understanding what light therapy is actually doing. Low level light therapy sends specific wavelengths of light into tissue. That light energy is absorbed by cells and may help support circulation, cellular repair, and the body’s natural response to inflammation. In practical terms, that can translate into joints that feel looser, less irritated, and more ready for movement.
People with osteoarthritis often look to light therapy for support around wear-and-tear joints like knees, hands, hips, and shoulders. People with inflammatory forms of arthritis may also explore it as a complementary option, although results can vary more depending on the condition, flare patterns, and treatment plan.
What light therapy may actually help with
Arthritis pain is rarely just pain. It often comes with swelling, tightness, reduced range of motion, and the habit of protecting a painful area until the rest of the body starts compensating. That is why a therapy that helps movement can matter just as much as one that helps discomfort.
Light therapy may help by easing local inflammation and improving tissue recovery around an affected joint. When pain comes down even a little, people often move more naturally. Better movement can support joint health, muscle engagement, and confidence. For active adults and athletes, that can mean getting off the sideline and back in the game. For someone managing chronic stiffness, it can mean making it through the day with less frustration.
There is also a timing advantage. Many people use light therapy before activity to loosen a stubborn area or after activity to calm it down. That flexibility makes it easier to fit into real life, whether your goal is gardening, training, or getting through a workday without paying for it later.
How it works without drugs or downtime
Low level light therapy is not heat therapy in the usual sense, and it does not rely on medication. It uses light energy to stimulate biological processes below the surface of the skin. Researchers have studied its effects on inflammation, blood flow, and cellular energy production, all of which are relevant when joints are under stress.
Think of it as support for the body’s repair and recovery systems. The body still has to do the work, but light therapy may help create a better environment for that work to happen. This is one reason it appeals to people who want a more natural approach. They are not looking to numb the problem for a few hours. They want to support better function and stay active longer.
That said, not every device is built the same. Wavelength, power, treatment time, and delivery method all matter. Some systems also use pulsed frequency delivery, which is designed to add another layer of stimulation beyond light alone. For consumers, that means results often depend on both the quality of the device and the consistency of use.
What the research suggests
The research around light therapy and arthritis is promising, though not perfectly uniform. Some studies have found benefits for pain relief and improved function, particularly in osteoarthritis and certain joint-related pain conditions. Other studies show more modest effects, which is common in pain research because arthritis itself is not one single experience.
That does not mean the therapy is weak. It means the outcome depends on several factors: the type of arthritis, the joint being treated, the stage of the condition, treatment settings, and whether the person is using it regularly enough to judge real results.
This matters because people often try a wellness tool once or twice and decide it does not work. Arthritis usually does not respond that quickly. Consistency is where the payoff tends to show up. A person with mild knee stiffness may notice a shift faster than someone with advanced joint degeneration or a whole-body inflammatory condition.
Who may benefit the most
People with mild to moderate joint pain often respond best, especially if they are still active and trying to stay that way. If your arthritis is making movement harder but not impossible, light therapy may be a strong fit because it can support your effort to keep moving before stiffness turns into a bigger cycle of limitation.
It may also be valuable for people who want to reduce how often they reach for pain relievers. That does not mean stopping prescribed treatment or ignoring medical advice. It means adding a supportive option that helps you manage symptoms in a safer, non-invasive way.
Athletes and highly active adults are another natural fit. Arthritis does not only affect older adults. Repetitive stress, old injuries, and heavy training can all contribute to joint pain over time. For this group, light therapy can be part of a performance-minded recovery plan, helping them stay more consistent with training and less reactive to aches that slow them down.
When the answer is yes, but with limits
If you are wondering can light therapy help arthritis enough to replace all other care, the honest answer is usually no. Arthritis is complex. Some cases involve cartilage loss, some involve active autoimmune inflammation, and many involve surrounding muscle tension and movement changes that need attention too.
Light therapy is best seen as part of a bigger strategy. That strategy may include strength work, mobility training, weight management, anti-inflammatory habits, physical therapy, and medical care when needed. The real win is not pretending one tool does everything. The real win is finding the right combination that helps you move with less pain and more freedom.
There are also moments when expectations need to stay realistic. If a joint is severely damaged, light therapy may still help reduce discomfort, but it may not restore the level of function you want on its own. If you are in the middle of a strong inflammatory flare, results may feel inconsistent. That does not make the tool useless. It just means context matters.
How to use it for the best chance of results
Consistency beats intensity. Regular sessions over time usually matter more than occasional use when pain spikes. Most people do better when they treat the affected area on a schedule and track how they feel over a few weeks rather than judging the experience after one day.
It also helps to match treatment to your routine. Use light therapy before activity if stiffness is your main issue. Use it after activity if swelling or soreness tends to build. Some people benefit from both. The goal is simple: make movement easier, recovery smoother, and pain less controlling.
Device quality matters here. A well-designed system should be simple enough for home use but powerful enough to support meaningful results. Life Light stands out in this category with pulsed frequency modulation, offering a more advanced approach for people who want natural pain support without slowing down their lives.
A smart way to think about light therapy for arthritis
Arthritis can make your world smaller one joint at a time. The right support can help you push back. Light therapy may not erase arthritis, but it may help reduce the pain, stiffness, and inflammation that keep you from doing what you want to do.
That is why this option keeps gaining attention. It speaks to people who want more than temporary relief. They want momentum. They want to stay independent, stay active, and live better without feeling trapped by the next flare-up. If that sounds like you, light therapy may be more than a trend. It may be one of the tools that helps you move brighter, stronger, and with more confidence.